
Your Body Is Communicating: Understanding Weak Pelvic Floor Treatment
Your Body Is Communicating: Understanding Weak Pelvic Floor Treatment
What Causes a Weak Pelvic Floor and What Treatment Options Are Available?
Weak pelvic floor treatment is more accessible than most people realize—and for many people, it does not require surgery or lifelong medication.
In fact, your body often starts sending signals years before symptoms become severe.
Most people simply don't realize their body is trying to tell them something.
Little leaks when you laugh.
A sudden urge to run to the bathroom.
The constant mental map of where the nearest bathroom is.
Waking up multiple times at night to urinate.
These symptoms are easy to brush off at first.
But they matter.
They are your body's way of communicating that the pelvic floor muscles are no longer as strong. coordinated, or as supported as they used to be.
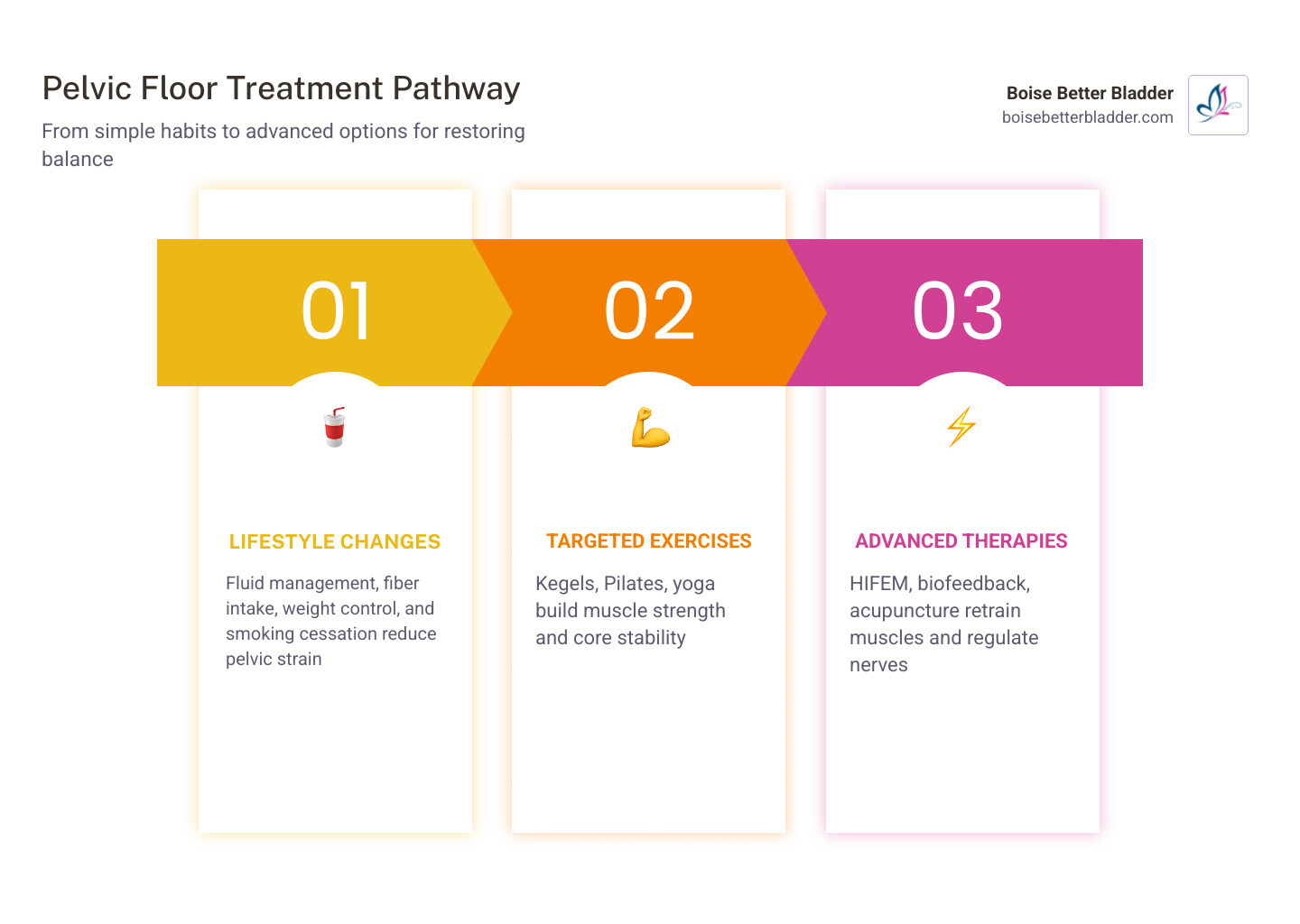
The good news is this: there are many treatment options available today—ranging from simple lifestyle changes to advanced therapies designed to restore strength and control to the pelvic floor.
Here is a quick overview of the most common options, from the least to the most involved.
Not sure where to start?
If you’re noticing bladder leaks, urgency, or changes in pelvic pressure, the most helpful first step is understanding why these symptoms are happening.
At Boise Better Bladder, we begin with a simple pelvic floor evaluation to identify which muscles and patterns may be contributing to your symptoms.
Once we understand the pattern, we can determine which weak pelvic floor treatment options may be most appropriate for your body.
➡Learn more about our pelvic floor evaluation process here
Understanding the Pelvic Floor
The pelvic floor is a group of muscles and connective tissue that forms a supportive hammock across the base of your pelvis. It holds your bladder, bowel, and uterus (or prostate) in place.
These muscles play an important role in everyday function. They help control urination and bowel movements, support sexual function, and even contribute to core stability and spinal support.
When this system is disrupted—by childbirth, aging, weight changes, hormonal shifts, or inactivity—your body begins sending signals.
Leaks when you laugh.
A feeling of heaviness or pressure.
Urgency that catches you off guard.
These are not signs of failure. They are patterns your body is communicating, asking for support.
The encouraging truth is this: women have roughly a 50% lifetime chance of developing pelvic organ prolapse, and pelvic floor dysfunction affects both men and women across all ages.
You are not alone—and the body has a remarkable capacity to restore balance when given the right guidance.
This guide walks through every layer ofweak pelvic floor treatment, from simple daily habits to advanced clinical options, so you can understand your body’s pattern and find the pathway that fits your life.
Lifestyle Changes
For mild symptoms, small lifestyle adjustments can sometimes reduce pressure on the pelvic floor and improve bladder function.
Examples include:
Fluid management
Increasing fiber intake
Weight loss
Smoking cessation
Reducing bladder irritants like caffeine and alcohol
These changes can absolutely be helpful.
But let's be honest–they do not actually rebuild weak pelvic floor muscles.
They may reduce irritation or symptom triggers, but they are often just one piece of the bigger picture.
Exercises
Pelvic floor exercises are commonly recommended as a first step in treatment.
Examples include:
Kegel exercises
Pilates
Yoga
Core strengthening
The goal is to improve support for the bladder, bowel, and pelvic organs by strengthening the muscles of the pelvic floor.
So yes, traditional exercise matters. But exercise alone is not always enough.
The challenge?
Many people either do Kegels incorrectly or do not perform enough repetitions to rebuild meaningful strength in the pelvic floor.
Physical Therapy
Pelvic floor physical therapists specialize in evaluating and retraining pelvic floor muscles.
Treatments may include:
Pelvic floor muscle training
Biofeedback
Manual therapy
Pelvic floor physical therapists are trained to assess how specific muscles are functioning and help patients improve coordination, strength, and control.
For some patients, this can be extremely helpful. For others, progress may be slow depending on the severity of muscle weakness.
Advanced Therapies
This is where treatment has become especially exciting.
In recent years, new advanced technologies have made it possible to strengthen the pelvic floor without surgery or invasive procedures.
Newer technologies are now available that can stimulate and strengthen the pelvic floor muscles in ways that go far beyond what most people can do on their own.
Examples include:
HIFEM technology (high-intensity electromagnetic stimulation)
Electrical stimulation therapies
Acupuncture to support nerve and muscle function
These advanced therapies stimulate the pelvic floor muscles and nerves to generate thousands of supramaximal contractions in a single session—something that would be nearly impossible to achieve with voluntary exercise alone.
Because of this, many people are relieved to learn that weak pelvic floor treatment has evolved dramatically in recent years. Modern, non-surgical options can now restore strength, improve control, and support real change..
This is one reason so many people are relieved to learn that weak pelvic floor treatment has evolved so much in recent years.
There are now modern, non-surgical options that can help restore strength, improve control, and support real change.
What I See in My Clinic
In my clinic, I meet women every week who have been quietly managing bladder leaks for years.
Many assumed it was simply part of aging.
Others were told that surgery would eventually be their only option.
But once we evaluate pelvic floor strength and begin strengthening those muscles properly, many patients are surprised by how much improvement is possible.
Some notice fewer leaks within a few weeks.
Others realize they are finally sleeping through the night again without waking up to use the bathroom.
These improvements happen because the pelvic floor muscles can often regain strength when they are properly stimulated and supported.
Most women simply didn’t know this kind of help existed.
Medical Interventions
When conservative therapies are not enough, physicians may recommend additional medical devices or medications.
These may include:
Pessaries to support pelvic organs
Medications that calm an overactive bladder/reduce urgency
Bladder training programs
These approaches can be useful, especially in more complex cases, but they often focus more on managing symptoms than restoring true pelvic floor strength.
Surgery
When conservative options have not worked, surgery may be considered.
Examples include:
Pelvic organ prolapse repair
Rectocele repair
Sling procedures for urinary incontinence
For some patients, surgery is appropriate and necessary.
But it is usually not the first step.
Many people are surprised to learn that there are other weak pelvic floor treatment options to explore before reaching that point.
The Body Works in Patterns
As a clinician, I often see patients who think of the pelvic floor as an isolated “problem area.”
But the body works in patterns.
The pelvic floor is actually part of a much larger support system that includes your diaphragm, deep abdominal muscles, and the small stabilizing muscles along your spine. Together, these structures form your core and help regulate pressure inside the abdomen.
When you cough, sneeze, laugh, or lift something heavy, this system should automatically coordinate to manage that pressure. If the pelvic floor is weak or unbalanced, that pressure has nowhere to go but downward—placing strain on the tissues meant to support the bladder, bowel, and pelvic organs.
Clinically, we often see two general patterns of pelvic floor dysfunction:
Underactive (Hypotonic) Pattern
The muscles lack enough strength or tension to properly support the pelvic organs. This can contribute to bladder leaks, stress incontinence, and pelvic organ prolapse.
Overactive (Hypertonic) Pattern
The muscles are too tight and cannot fully relax. This may cause pelvic pain, difficulty emptying the bladder, or discomfort during intimacy. Over time, muscles that stay constantly tight can actually become weak as well.
Understanding these patterns is the first step toward restoring balance and strengthening the pelvic floor.
Recognizing the Signals
Your body isn't failing you–it's communicating.
When these muscles lose strength or coordination, the body begins sending messages.
Urinary leakage: A few drops when you cough, laugh or exercise.
Sudden urgency: The feeling that you need to run to the bathroom immediately. And sometimes you can't!
Pelvic heaviness or pressure: A heavy sensation that feels like something is "out of place".
Pelvic organ prolapse: When the bladder, uterus or your bowels shift downward into the vaginal canal.
Bowel difficulties: This includes constipation or even fecal incontinence.
Changes in sexual function: This can include decreased sexual sensation, discomfort, erectile dysfunction, and difficulty having an orgasm.
These symptoms are incredibly common, yet many people assume they are simply a normal part of aging.
The good news is that recognizing these signal early allows us to explore non-invasive weak pelvic floor treatment options long before surgery becomes necessary.
First-Line Weak Pelvic Floor Treatment and Lifestyle Shifts

When we begin addressing a weak pelvic floor, we often start by supporting the body’s natural rhythms. Small, thoughtful shifts in your daily routine can significantly reduce the "load" on your pelvic muscles, allowing them a chance to heal and strengthen.
Supporting Natural Rhythms
The way we treat our digestive and urinary systems directly impacts pelvic health.
Fluid Management: Many people with leakage stop drinking water. This is actually counter-productive. Dehydration makes urine more concentrated, which irritates the bladder lining and increases urgency. Aim for 6 to 8 glasses of water a day.
Caffeine and Alcohol Reduction: These are known bladder irritants. Caffeine, in particular, can act as a diuretic and a stimulant, making the bladder "twitchy."
Prioritizing Fiber: Chronic straining due to constipation is one of the leading causes of pelvic floor weakness. A high-fiber diet helps ensure bowel movements are easy to pass, protecting the hammock from unnecessary downward pressure.
Smoking Cessation: Chronic coughing—often seen in smokers—puts immense, repetitive strain on the pelvic floor.
Weight Management: Excess weight, particularly in the abdominal area, increases the constant pressure on the pelvic organs.
Bladder Retraining
Our bladders are often conditioned by our behavior. If you go "just in case" every time you see a bathroom, you are teaching your bladder to signal for emptying at low volumes.
The average person should only need to void 4 to 6 times during the day. We encourage patients to "ignore" the first small habitual urge and wait until the bladder is actually full. This helps retrain the nervous system and the bladder wall to hold more comfortably.
“Symptoms are signals.”
Correcting the Pattern: Weak Pelvic Floor Treatment Through Exercise
Exercise is a cornerstone of weak pelvic floor treatment, but it must be done with precision. Simply "squeezing" isn't always enough; we must re-educate the muscles to work in the correct sequence.
The Precision of Kegel Exercises: Developed in the 1940s, Kegels involve lifting and squeezing the pelvic muscles. To do them correctly, imagine you are trying to stop the flow of urine and prevent passing gas simultaneously.
Quick Squeezes vs. Long Holds: Your pelvic floor contains different types of muscle fibers. "Quick flicks" (1-2 second squeezes) help with the fast reaction needed when you cough. "Long holds" (aiming for 10 seconds) build the endurance needed to support your organs throughout the day.
Core Stability: Because the pelvic floor is part of the core, we often recommend Pilates and Yoga. These disciplines focus on deep stability and breathing, which helps the pelvic floor integrate with the rest of the body.
Proper Lifting Technique: Never hold your breath when lifting. Instead, "exhale on the exertion" and gently engage your pelvic floor before you lift. This protects the "hammock" from sudden pressure spikes.
When Lifestyle Shifts Need Further Support: Exploring Deeper Pathways
Sometimes, even with diligent lifestyle adjustments and exercise, the body's patterns require a more focused approach to restore balance. This is especially true if the connection between the brain and the muscles has been weakened by trauma, surgery, or years of dysfunction.
In some cases, the signal between the brain and the pelvic floor becomes weak or uncoordinated—almost like a radio station filled with static. This is where specialized, targeted interventions can offer profound support, helping to re-establish optimal muscle function and nervous system regulation. Our goal is always to empower your body's innate healing capabilities by clearing that static and strengthening the signal.
A Modern Approach to Weak Pelvic Floor Treatment in Boise
At Boise Better Bladder, we believe that the most effective healing happens when we look at the root cause. We blend ancient clinical wisdom with modern, FDA-approved science to address the patterns of pelvic floor imbalance.
Our programs are entirely non-invasive and surgery-free. We don't just want to "fix" a symptom; we want to restore the integrity of the system.
HIFEM Technology: Deep Muscle Retraining
High-Intensity Focused Electromagnetic (HIFEM) technology is a breakthrough in weak pelvic floor treatment. While a person might struggle to perform a few dozen Kegels correctly at home, a single 30-minute session with our HIFEM technology induces the equivalent of 25,000 Kegels.
This isn't just about strength; it's about re-education. The technology forces the muscles to contract and relax in a perfect pattern, "re-mapping" the neural pathways between your brain and your pelvic floor. It deeply activates the tissue, restoring muscle tone and significantly improving bladder control without the need for internal exams or invasive procedures.
The Balancing Power of Acupuncture
Acupuncture is an ancient practice that excels at harmonizing the nervous system. From a clinical perspective, we use it to:
Improve Circulation: Bringing fresh blood and nutrients to weakened pelvic tissues.
Reduce Muscle Tension: Helping "hypertonic" or tight muscles finally let go so they can function properly.
Regulate the Nervous System: Calming the "fight or flight" response that often contributes to bladder urgency and pelvic pain.
By combining the high-tech muscle activation of HIFEM with the systemic balancing of acupuncture, we offer a unique pathway to healing that addresses both the physical muscles and the energetic and nervous system patterns that govern them.
Personalized Care and Clinical Clarity
Every body is different. We don't believe in one-size-fits-all protocols. We provide personalized care plans tailored to your specific symptoms and history. Our goal is to provide you with clinical clarity—helping you understand exactly why your body is sending these signals and how we can work together to resolve the root cause.
“Your body isn’t failing you.”
Frequently Asked Questions about Pelvic Floor Health
How is a weak pelvic floor diagnosed?
Diagnosis typically begins with a thorough history and a physical evaluation. As clinicians, we look for the specific patterns of how your body is holding tension or where it has lost its supportive tone. Specialists may use various tools, including:
Physical Exam: Checking for signs of prolapse or muscle weakness.
Bladder Diaries: Tracking fluid intake and voiding patterns.
Advanced Imaging: In some cases, a Pelvic Floor MRI or ultrasound may be used to visualize the support structures.
Urodynamic Testing: To measure how well the bladder holds and releases urine.
Is pelvic floor treatment different for men and women?
While the anatomy differs, the principles of weak pelvic floor treatment are very similar because the underlying patterns of dysfunction often overlap.
Women: Treatment often focuses on recovery after childbirth, changes around menopause, and symptoms associated with pelvic organ support.
Men: Issues often arise after prostate surgery, chronic heavy lifting, or long periods of sitting. Men can experience leakage and erectile dysfunction as a result of pelvic floor weakness.
In both cases, the best plan is the one that matches your pattern: how your muscles coordinate, how your breathing and core manage pressure, and how your nervous system is regulating urgency, tone, and recovery.
When should I seek professional medical help for symptoms?
If your symptoms are affecting your quality of life, it is time to seek help. You should not have to plan your life around the nearest bathroom or avoid activities you love because of fear of leakage. Specifically, seek help if you notice:
A visible bulge or feeling of a lump in the vaginal area.
Difficulty starting urination or feeling that the bladder is not empty.
Pain that interferes with daily life or intimacy.
Incontinence that requires the use of pads.
If you would like a clear, non-invasive starting point, you can also learn more about our approach here: More info about how it works
Conclusion
Your body is always communicating. Those leaks, that heaviness, and that urgency are not failures—they are signals that your internal support system is out of balance.
By understanding these patterns and addressing the root cause through a combination of lifestyle shifts, targeted exercise, and advanced non-invasive therapies, you can restore your body's natural equilibrium. At Boise Better Bladder, we are here to provide the clinical expertise and supportive care needed to help you reclaim your comfort and confidence.
The journey to a stronger, more resilient you starts with a single step toward understanding.
The Bigger Message
If you are dealing with leakage, urgency, pelvic pressure, or changes in bladder control–it does not mean that your bladder is broken.
Your body is communicating with you.
Pelvic floor weakness is incredibly common—especially after pregnancy, childbirth, hormonal changes, or simply as part of the natural aging process.
But common does not mean untreatable.
Modern, non-surgical weak pelvic floor treatment options can strengthen the muscles that support the bladder and pelvic organs instead of simply managing symptoms.
And when the pelvic floor becomes stronger again, something wonderful happens.
People regain confidence.
They sleep through the night.
They stop worrying about where the nearest bathroom is.
Most importantly, they begin engaging in life again without fear or embarrassment.
The first step is simply understanding what your body is telling you.
Book an Appointment