
The Anatomy of a Signal: Why Leaks Happen After Childbirth
The Anatomy of a Signal: Why Leaks Happen After Childbirth
Postpartum incontinence help starts with understanding that bladder leaks after having a baby are common — but they are not something you simply have to accept.
Quick answers for postpartum bladder leaks:
Start Kegel exercises as soon as they feel pain-free after delivery
Avoid bladder irritants like caffeine, alcohol, and carbonated drinks
Stay hydrated — concentrated urine irritates the bladder and worsens leaks
Eat fiber-rich foods to prevent constipation and reduce pelvic strain
See a specialist if leaks persist beyond 6–8 weeks postpartum
Ask about pelvic floor therapy — it's more effective than Kegels alone
Consider advanced options like HIFEM technology or acupuncture if first-line approaches haven't worked
Around 1 in 3 women experience urinary incontinence after having a baby. Leaking when you laugh, sneeze, cough, or lift your newborn is one of the most common — and least talked about — parts of early motherhood.
But here is what matters: common does not mean normal. And it certainly does not mean permanent.
Many women are told to simply do their Kegels and wait it out. Some are told it is just part of having children. Others eventually hear that surgery is their only real option.
None of that is the full picture.
Your body isn't failing you. It is sending a signal — one that deserves to be understood and properly addressed.
What you're experiencing after childbirth reflects real, measurable changes in your pelvic floor muscles, nerve pathways, and hormonal environment. These are patterns that can be identified, treated, and in most cases, meaningfully improved.
I'm Dr. Kimberly Thompson, DACM, L.Ac., and I've spent years working with women seeking genuine postpartum incontinence help — many of whom came to me after Kegels, pelvic PT, and medications had already let them down. My approach combines advanced HIFEM technology, acupuncture, and whole-body care to address the root cause, not just the symptoms. In this guide, I'll walk you through exactly what's happening in your body and what actually works.
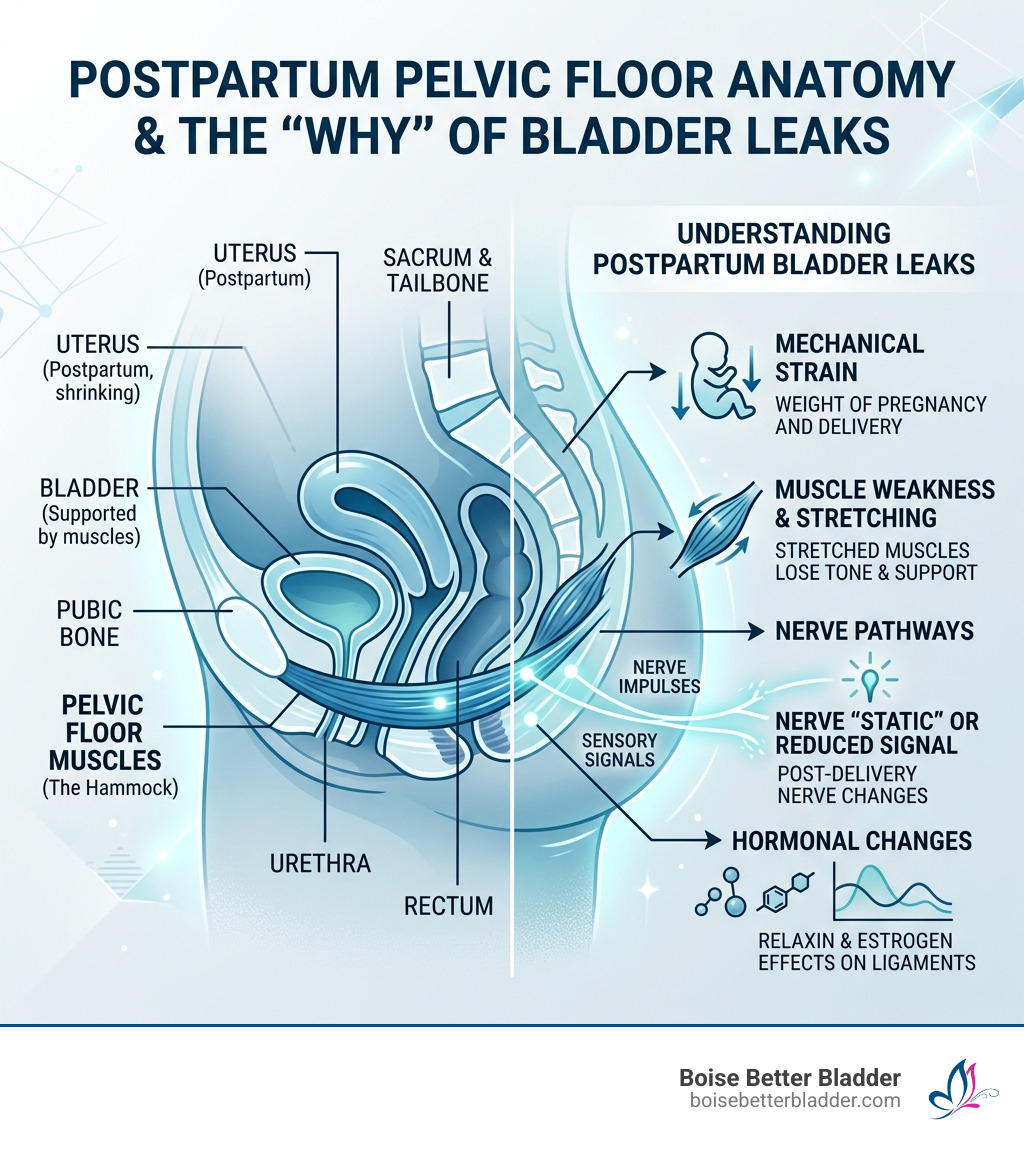
To find the right postpartum incontinence help, we must first understand the "why." Your body works in patterns, and the pattern of postpartum leakage is often a combination of mechanical strain and neurological "static."
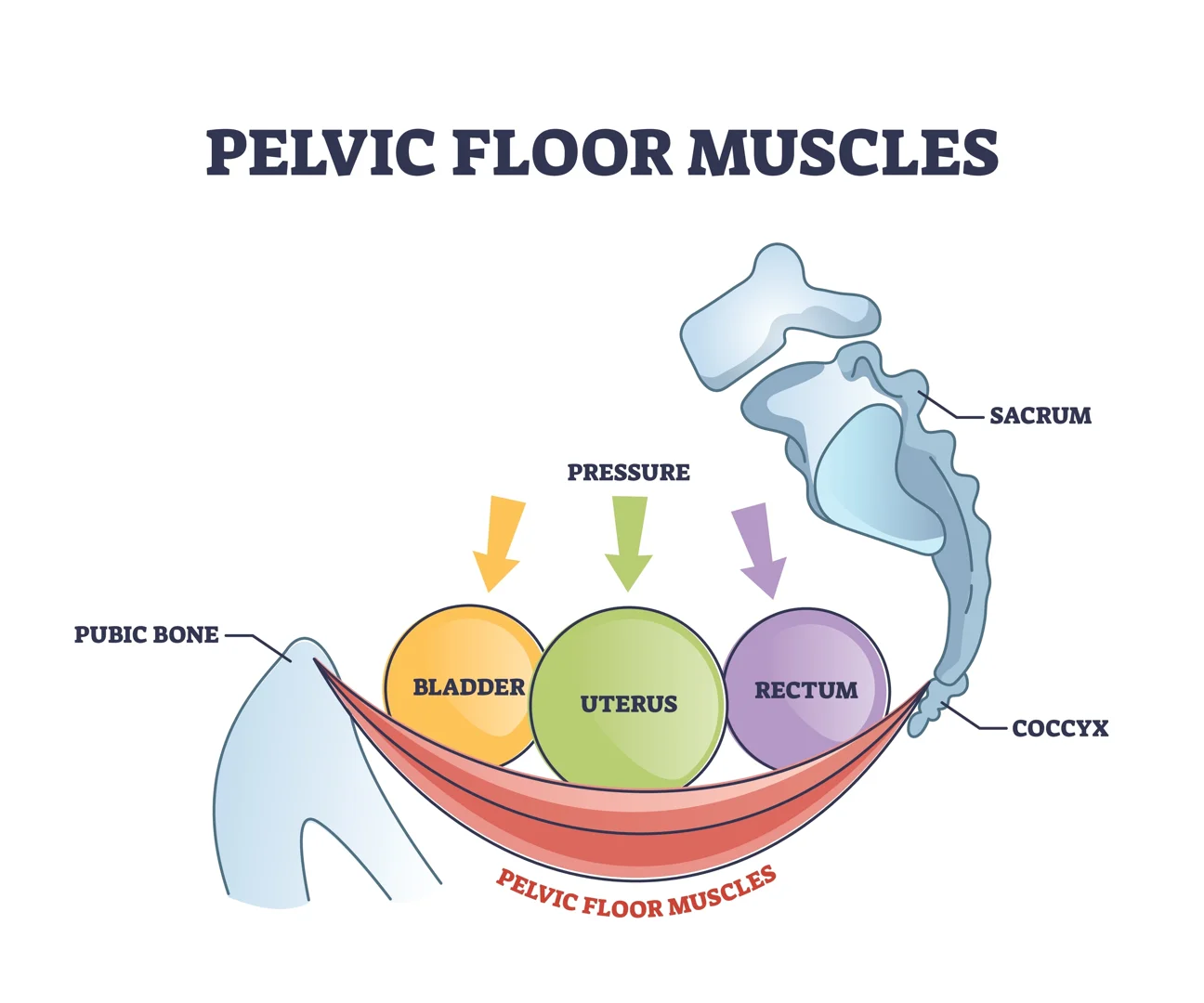
During pregnancy, your pelvic floor muscles—the hammock-like structure that supports your bladder, uterus, and bowel—carry significant weight. This constant pressure, combined with the hormone relaxin which softens ligaments for birth, can lead to significant stretching.
Research published in Nature Reviews Urology highlights that pregnancy and childbirth involve anatomical and physiological changes that can negatively affect the urinary-continence mechanism. It isn't just about "weakness"; it's about a disruption in how these tissues support the urethra.
Key factors include:
The Pudendal Nerve: During a long or difficult vaginal delivery, the pudendal nerve can be stretched or compressed. This nerve is the primary "telephone wire" between your brain and your pelvic floor. When it’s irritated, the signal to "hold" may arrive too late or too weak.
Levator Ani Muscle Strain: This is the major muscle of the pelvic floor. Pushing, especially prolonged pushing or the use of forceps and vacuums, can cause micro-tears or significant stretching in this muscle.
Hormonal Shifts: After delivery, there is a steep drop in estrogen. Estrogen is vital for maintaining the thickness and elasticity of the tissues around the bladder and urethra. When estrogen is low (especially if you are breastfeeding), these tissues can become thin and less capable of creating a tight seal.
Symptoms are signals. If you are leaking, your body is telling you that the communication between your nerves and muscles has been interrupted.
Identifying Your Pattern: Stress, Urge, and Mixed Incontinence
Not all leaks are created equal. Identifying your specific pattern is the first step toward effective postpartum incontinence help.
Stress Incontinence
This is the most common type, affecting roughly 30% of women postpartum. It occurs when physical pressure (stress) is placed on the bladder. If you leak when you:
Laugh or sneeze
Cough or jump
Lift your baby or a car seat
Exercise
...you are likely dealing with stress incontinence. This is usually a sign that the "door" (the urethral sphincter) isn't staying shut against sudden pressure because the supporting muscles are too stretched or tired.
Urge Incontinence
This pattern is less about muscle strength and more about nervous system communication. You might feel a sudden, intense "gotta go" sensation that you can't suppress, leading to a leak before you reach the bathroom. This often happens because the bladder muscle (the detrusor) is overactive or receiving "false alarms" from the nerves.
Mixed Incontinence
Many women in our Boise and Meridian communities experience a combination of both. You might leak when you sneeze and feel like you can't make it to the bathroom in time.
Symptom Stress Incontinence Urge Incontinence Trigger Physical movement (cough, lift) Sudden, intense urge Amount of Leak Usually small drops or a squirt Can be a large volume Warning No warning, happens with the movement Sudden "gotta go" feeling Frequency Depends on activity level Often high (frequent trips)
Holistic Postpartum Incontinence Help: Restoring the Pelvic Pattern
At Boise Better Bladder, we look at the body as an integrated system. We aren't just looking at a "weak muscle"; we are looking at how the nerves, circulation, and muscles coordinate.
How It Works involves a multi-layered approach. We want to restore the "brain-floor connection." If the nerves aren't firing correctly, no amount of traditional exercise will fix the problem.
The Role of Circulation and Breath
The pelvic floor doesn't work in isolation. It is the bottom of your "core canister," which includes your diaphragm at the top. When you breathe, your pelvic floor should move in rhythm with your diaphragm.
Diaphragmatic Breathing: Inhaling should allow the pelvic floor to gently expand; exhaling should allow it to naturally lift.
Pelvic Circulation: Healing requires blood flow. Acupuncture is a powerful tool here, as it helps regulate the nervous system and encourages micro-circulation to the pelvic tissues, providing the nutrients needed for nerve regeneration and muscle repair.
Lifestyle Adjustments for Postpartum Incontinence Help
Small changes in your daily routine can significantly reduce the load on your pelvic floor while you are healing.
Mindful Hydration: Many women stop drinking water to avoid leaks, but this backfires. Dehydration leads to concentrated urine, which irritates the bladder lining and triggers more urgency. Aim for steady hydration throughout the day, but perhaps limit fluids two hours before bed.
Identify Irritants: Caffeine (coffee/tea), alcohol, carbonated drinks, and spicy foods are common bladder irritants. They act like "itchy wool" for your bladder.
Fiber and Constipation: Straining to have a bowel movement is one of the hardest things you can do to a postpartum pelvic floor. Ensure you are getting enough fiber and consider a stool if needed to keep things moving easily.
When to Seek Professional Postpartum Incontinence Help
While some improvement is expected as your body heals in the first few weeks, you shouldn't wait forever. The "6-week checkup" is a great time to bring this up with your provider.
If you are experiencing:
Leakage that hasn't improved by 8 weeks postpartum.
A feeling of heaviness or "something falling out" (potential prolapse).
Pain during intercourse.
Frequent "false alarms" where you run to the bathroom but very little comes out.
It is time for a specialized evaluation. Your body isn't failing; it just needs a more targeted therapeutic pathway than "wait and see."
Frequently Asked Questions about Postpartum Bladder Control
How long does postpartum incontinence typically last?
For many, symptoms resolve within the first 6 to 12 weeks as the uterus shrinks and hormones begin to stabilize. However, research shows that only about 5% of women have ongoing issues a year later if they seek help. If symptoms persist beyond 6 months, they are unlikely to go away on their own. This is often because the body has "learned" a dysfunctional movement pattern or the nerve communication remains dampened.
Is the risk different for a C-section versus a vaginal birth?
There is a common misconception that a C-section "protects" the pelvic floor. While women who deliver naturally have a 50% greater chance of developing incontinence because of the direct stretching of the birth canal, pregnancy itself is a major factor. Carrying a baby for nine months puts immense strain on the pelvic floor regardless of the exit route. C-section moms also have to contend with abdominal scar tissue, which can change how the core muscles support the bladder.
How do I perform Kegel exercises correctly for pelvic floor strengthening?
Many women do Kegels incorrectly by "bearing down" or holding their breath.
Isolate: Imagine you are trying to pick up a blueberry with your vagina or stop the flow of urine (don't actually do this while peeing, as it can confuse the bladder).
Lift: It's not just a squeeze; it's an upward lift toward your belly button.
Relax: This is the most important part! A muscle that can't relax can't contract effectively. Ensure you fully let go between reps.
Quality over Quantity: Doing 10 correct, mindful lifts is better than 100 fast, shallow ones.
For those who find Kegels difficult or ineffective, The Ideal Exercise Routine for Postnatal Incontinence often requires professional guidance to ensure you aren't accidentally straining.
Conclusion: A Path Toward Lasting Restoration
At Boise Better Bladder, we serve women in Boise, Meridian, and Eagle who are tired of "just dealing with it." We understand that the transition to motherhood is demanding enough without the added anxiety of bladder leaks.
Our signature program is designed to be the "easy button" for your pelvic floor. By using FDA-cleared HIFEM technology, we can trigger the equivalent of 25,000 Kegel exercises in just 30 minutes. This isn't about "working harder"; it's about using technology to jumpstart the muscle and nerve coordination that pregnancy and birth disrupted.
For most of our patients, this HIFEM treatment alone has produced amazing results. If your case is severe, we can combine this with holistic acupuncture, and we address the root cause—improving circulation, calming the nervous system, and restoring the body’s natural patterns.
You don't have to choose between surgery, medications, or years of pads. There is a path to feeling like yourself again—confident, dry, and free to enjoy your new baby.
If you’re ready to stop managing symptoms and start restoring function, we invite you to Book an Appointment for an evaluation. Let’s help your body find its way back to balance.